“I was so excited when I massaged my breast and the first drops of milk came out”, says Caroline, a mother with an adopted baby. “It was only a few drops but my body had made them!” Caroline is one of an increasing number of adoptive mothers who are breastfeeding their babies.
 There are many advantages to breastfeeding an adopted baby, says Jean Ridler, an International Board Certified Lactation Consultant (IBCLC). Mothers who are unable to give birth to their own babies often feel that their bodies have failed them. Breastfeeding their adopted babies reminds them that their bodies can do it right and that they can be mothers in every sense of the word.
There are many advantages to breastfeeding an adopted baby, says Jean Ridler, an International Board Certified Lactation Consultant (IBCLC). Mothers who are unable to give birth to their own babies often feel that their bodies have failed them. Breastfeeding their adopted babies reminds them that their bodies can do it right and that they can be mothers in every sense of the word.
The physical closeness of the breastfeeding experience also helps the mother to bond with her new baby, and the hormones that are made when breastfeeding — prolactin and oxytocin, have been called the “mother-love” hormones. Prolactin increases nurturing behaviour, and the hormone oxytocin (also released by both partners during love-making) gives us the desire to cuddle with our partner, or in this case, the baby.
How mothers make milk
To understand how adoptive moms can breastfeed, it helps to understand the physiology of breastfeeding. During pregnancy, the mother has elevated levels of prolactin and oestrogen, which prepare her body to breastfeed. At the same time the baby’s placenta makes large amounts of progesterone, which maintains the pregnancy and prevents the breastmilk from coming in before the baby is born.
After birth, when the placenta comes away, the mother’s progesterone levels drop suddenly, and her body gets the message, “The baby has been born, make milk”. That is why, on about the third day, her milk comes in with a whoosh (as many mothers know). But from then on, it is the baby who regulates the milk supply by sucking, and if there is no baby to suck, or if she offers bottles of formula, the mother’s milk supply will soon dry up.
So the key to having a milk supply for your baby (adopted or not) is how much the baby sucks at the breast. As the baby nurses, messages are sent to the pituitary, which secretes prolactin and oxytocin, telling the body how much milk to make for this particular baby’s needs. So frequent sucking is very important says Jean, and very important indeed is making sure that the breast is emptied as much as possible at each feed, so that the body gets the message to make more milk.
In the old days, pumping (to simulate the baby sucking) was the only method we knew of to start a milk supply without a pregnancy, and so mothers who wished to breastfeed their adopted babies, would optimally need to start pumping months before the baby was born. It could be done, and some mothers did well, though it was hard work. Today we know how to use hormones to make the mother’s body think she is pregnant, and to enlarge and prepare the breasts for breastfeeding. This makes it a lot easier, though Jean says that if she found a mom who didn’t want to use them, she would still be happy to support her.
When baby arrives
Adopting mothers often don’t know when they will be getting their baby. Some moms have to wait for several years, while others are suddenly given a few weeks (or even days) notice. But lactation consultants have a protocol to deal with all these situations, and Jean says that with the right help, any woman (even if she doesn’t have a uterus or ovaries) can breastfeed an adopted baby. She emphasises the right help and says that it is important to find a lactation consultant (preferably an IBCLC) with experience.
In the ideal situation according to Jean, the mother knows about nine months before she will be getting the baby, and that is when she can begin to take the hormones. She will be given oestrogen and progesterone (found in birth control pills) and also an anti-nausea medication, domperidone, which has the side effect of creating prolactin as well. Within about a month, there will be a noticeable enlargement of her breasts.
About four weeks before she is due to get the baby, the hormones are stopped, and the withdrawal of the progesterone makes her body think she has given birth. The domperidone is continued to increase her prolactin, and she can also use some herbs such as Fenugreek and Blessed Thistle if she wishes. At this point she needs to start pumping, and Jean says it is important to have a high-grade electrical pump for this purpose. The mother will probably start producing milk right away, sometimes just a few drops, but sometimes quite a lot. This can be frozen and stored to use when the baby arrives.
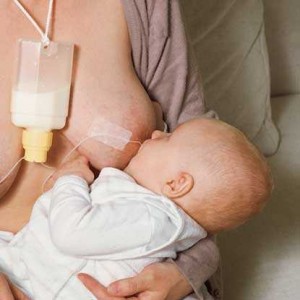
The mother’s milk increases more gradually if there hasn’t been a pregnancy, so the adopting mother will, at least for some time, need to supplement using an SNS (supplemental nutrition system). This is a small container of formula or stored breastmilk that she wears around her neck. A thin tube running down from this device is placed against the mother’s nipple (it can be secured with a band-aid if she wishes) and ensures that while the baby is sucking, it is also getting enough food. The SNS is designed in such a way that the breast is emptied first, so if the baby starts leaving some of the milk behind in the SNS after a while, it is a good indication that the mother’s supply is increasing.
Getting the new baby properly positioned at the breast is the first priority, says Jean. The mother’s lactation consultant will help her with this. Feeding frequently enough is also important, and the baby will need 10 to 12 feeds in a 24-hour period. Because prolactin levels are higher at night, night-time feeding has advantages, and keeping the baby in close proximity to the mother’s body at night makes this easier. Offering the baby a bottle will deprive the breast of essential stimulation, so it is important that all sucking takes place at the breast, and that the mother avoids the use of dummies (pacifiers) or bottles.
But some mothers don’t know that they will be getting the baby till a few days before it arrives, and Jean says that such mothers can breastfeed too. Like all adoptive mothers, they will need to invest in an SMS (supplemental nutrition system), though unlike the prepared mothers, their baby will be totally dependent on the formula it supplies at the beginning, until the sucking of the baby begins to bring in the mother’s own milk. Caroline was one such mother.
Caroline’s Story
“We were told on the Friday that there was a baby for us, and that we could collect her on the Monday”, says Caroline, who adopted her little girl through a private adoption agency. Two weeks before that they were told by the agency that they had been approved, and that the next phone call would be to tell them that there was a baby for them.
Caroline was referred to Jean Ridler, and knowing that they didn’t have much time, Jean put them onto what is known as the “accelerated protocol”. Since there wasn’t enough time for Caroline to go onto the full hormone treatment, she was given a short course of hormones and put onto domperidone to get her body to make prolactin. Jean also went round to her home and showed her a video on how to breastfeed, and demonstrated how to use the SNS.
But things still went faster than they had expected. They were only one week into the treatment when they were told they could come in on the Monday and collect their baby. When the baby arrived Caroline thought, “This will be easy, I saw the video, and I know what to do”. So she put some formula into the SNS and tried to latch the baby onto the breast. “Then I realized that I didn’t even know how to hold her in the right position”, she said.
So she phoned Jean and Jean came over immediately. “I was so grateful to her”, says Caroline, “She put the baby into the proper position, my baby latched on, and we were away. It was just so beautiful!” Everything went smoothly from then on. Knowing that Caroline was going to breastfeed, the agency had fed the baby every two hours to get her used to frequent feedings. Night times were a bit hectic, Caroline says, as her baby fed three or four times every night, but it helped her milk to come in quicker.
About a month after the baby started sucking at the breast, Caroline’s milk really started to come in. “My breasts started to feel a bit lumpy”, she says, “and as I rubbed one of the lumps, some milk came out. It felt amazing. My milk increased more and more with time, till finally, after three months it would squirt out in a stream. I increased my supply by feeding her throughout the day, whenever she was willing to suck.” Caroline breastfed her baby till the SNS broke at 9 months. She also continued to take the domperidone. “I didn’t mind, as long as I was feeding my baby”, she said, “It was wonderful”.
Jean emphasises that there are differences between breastfeeding an adopted baby and one to whom the mother has given birth. In the latter case, the mother’s milk will quickly catch up to 100% of the baby’s needs if the baby is allowed to suck frequently enough. With an adoptive mother, the milk supply will increase more slowly, reaching full capacity for that mother, about three months after she starts nursing the baby.
The full capacity of milk production in an adopting mother will also vary from mother to mother. It could be 100% (in which case she won’t need the SNS anymore). But even it if it just 80% or even only 50% of what the baby needs, Jean says, that isn’t what is important. What is important is that the mother is feeding the baby and sharing all the loving and closeness that goes with that. It’s best for the baby and the moms feel really good about the fact that they are able to do it.
An adoptive mother who wishes to breastfeed should have professional assistance. Ask at your nearest maternity hospital or clinic to be referred to a fully qualified International Board Certified Lactation Consultant (IBCLC), or your nearest La Leache League may be able to refer you to someone who specialises in breastfeeding adopted babies.
Written by Pat Törngren © 2012
(Article checked by Jean Ridler, IBCLC)
Suggested reading:
- “Breastfeeding an Adopted Baby and Relactation”, by Elizabeth Hormann, (La Leche League, USA, 2007)
- “Breastfeeding Made Simple: Seven Natural Laws for Nursing Mothers”, by Nancy Morbacher and Kathleen Kendall–Tackett (New Harbinger, USA, 2005)
Find more breastfeedinginformation on this helpful internet site: AskLenore.com

Someone wrote in to know if she could breastfeed an adopted baby even though she has had a hysterectomy. Yes you can — you don’t need to have either a uterus or ovaries to be able to breastfeed. In fact even men can produce milk if they wish to — though most don’t!
Women who don’t have a uterus or even ovaries can breastfeed this way, and there is no age limit either. In some cultures grandmothers “relactate” so that they can feed their grandchildren if the mother has to go back to work, or if she has triplets or even more babies all at once, and it would help to have two ‘mothers’ feeding the babies.
Can a baby suck on the breast of a woman who hasn’t given birth and milk would start dripping?
Hi Stevens, I am not sure what you are asking. I presume you have read the article. If so you will know that if a baby sucks on a mother’s breast, she will start making milk, even if the mother has never been pregnant, or doesn’t even have a uterus or ovaries. But it is hard to get a baby to keep sucking while getting nothing, which is why we use the SNS, so that the baby is getting milk and is encouraged to go on sucking. If you are asking if the other breast would start “dripping”, I guess once the mother has got a good milk supply established, then if she had a strong let-down, milk might drip from the breast the baby wasn’t sucking on.
In fact even men can lactate and feed a baby (and there are records of it having happened). The only problem is that the baby has to have enough breast to get into its mouth, so men who want to lactate would have to have hormone injections to make the breasts grow, go onto the domperidone (or one of the other medications that cause lactation in females and males) use the SNS and have the baby start to suck. I’m not advocating it, just mentioning that it has been done by a few fathers when the baby’s mother died. I’m not sure who fed the baby in the meanwhile, because it takes quite a while to get a milk supply established except in mothers who have just given birth.
Wow. I never thought breast feeding is possible with women who did not bear a child. Hmmm, interesting. Nice read.
Thank you so much for this article!
I would like to know if it is possible for an adoptive mother to lactate sufficiently with the use of and SNS from the day she meets her baby BUT with no use of hormone treatment at all.
Hi Elena, Yes is is possible to breastfeed an adopted baby without taking hormones. The procedure is to get a good quality pump and start stimulating your supply by pumping. It can take around six months (for some women longer and for others, shorter.) As your milk starts to come in, you can freeze it to have something to give to the baby in the SNS besides formula when baby arrives. The natural remedies mentioned in the article can also help.
I was able to breastfeed our third child who joined our family through adoption. It was a wonderful experience!
I had been pumping regularly for a few months in preparation for an infant to arrive. I also took domperidome. I quit pumping in November after an adoption failed to go through. Then we got the call out of the blue at 10 pm. We picked up our one-day old baby the next afternoon. My lactation consultant came over the following day and got us all set up with the supplemented and formula. He latched on after a few tries.
By about 3 months, I was providing about 80% of his nutrition through my breast milk. However, he would never nurse without the supplementer! Around 7 months, he started to fuss and would only nurse while in the sling and in a quiet setting. My older sister, who had nursed all 3 of her kids, commented that her kids all did the same thing when they were 9 months old and we’re getting ready to walk. Well, the little guy weaned himselF from the breast and started walked across the room to Grandma a day before he turned 8 months old!
So glad I had that time to nurse a little one.
Hi Deb, I am so happy for you that you managed to get assistance and succeeded so beautifully in breastfeeding your adopted baby. I love reading success stories like this and producing 80% of the milk your baby needed is awesome!
You said you were on Domperidone at first, and then stopped when an adoption didn’t go through. Then a baby arrived out of the blue. Was that much later? I hope you don’t mind me asking, but I am just curious about how long that was after you stopped the Domperidone and pumping (if you stopped the latter).
Also wondering if you went onto the Domperidone again when your little surprise arrived so suddenly. The reason I ask is that recently a mom asked me if she could build up a supply for adopting a baby without the domperidone, and I told her she could but it would take longer. So this information would be very helpful.
Isn’t it amazing! I never knew this was possible! I had such an amazing experience breastfeeding our son. It’s so nice to know an adoptive mama can have that same bonding experience! Motherly instincts are AMAZING! YOU GO MAMA!!!